advertiser-bcce
 From the pages of the Baby & Child Care Encyclopedia: Chapter 8, Safety and First Aid
From the pages of the Baby & Child Care Encyclopedia: Chapter 8, Safety and First Aid
If you’ve ever experienced the moment of panic when your child is choking on something, you know how helpless you can feel. But knowing how to help, no matter your child’s age, will go a long way to making sure you’re prepared.
CHOKING BABY (UNDER ONE YEAR)
Note If a baby is too heavy or large to support with your forearm, treat the baby as you would treat a choking child.
- If a baby is coughing or gagging, the choking is mild. Do not interfere.
- If the baby is making high-pitched noises, wheezing, can no longer make a sound or becomes too weak to cough, have someone call EMS and care for the baby.
Care
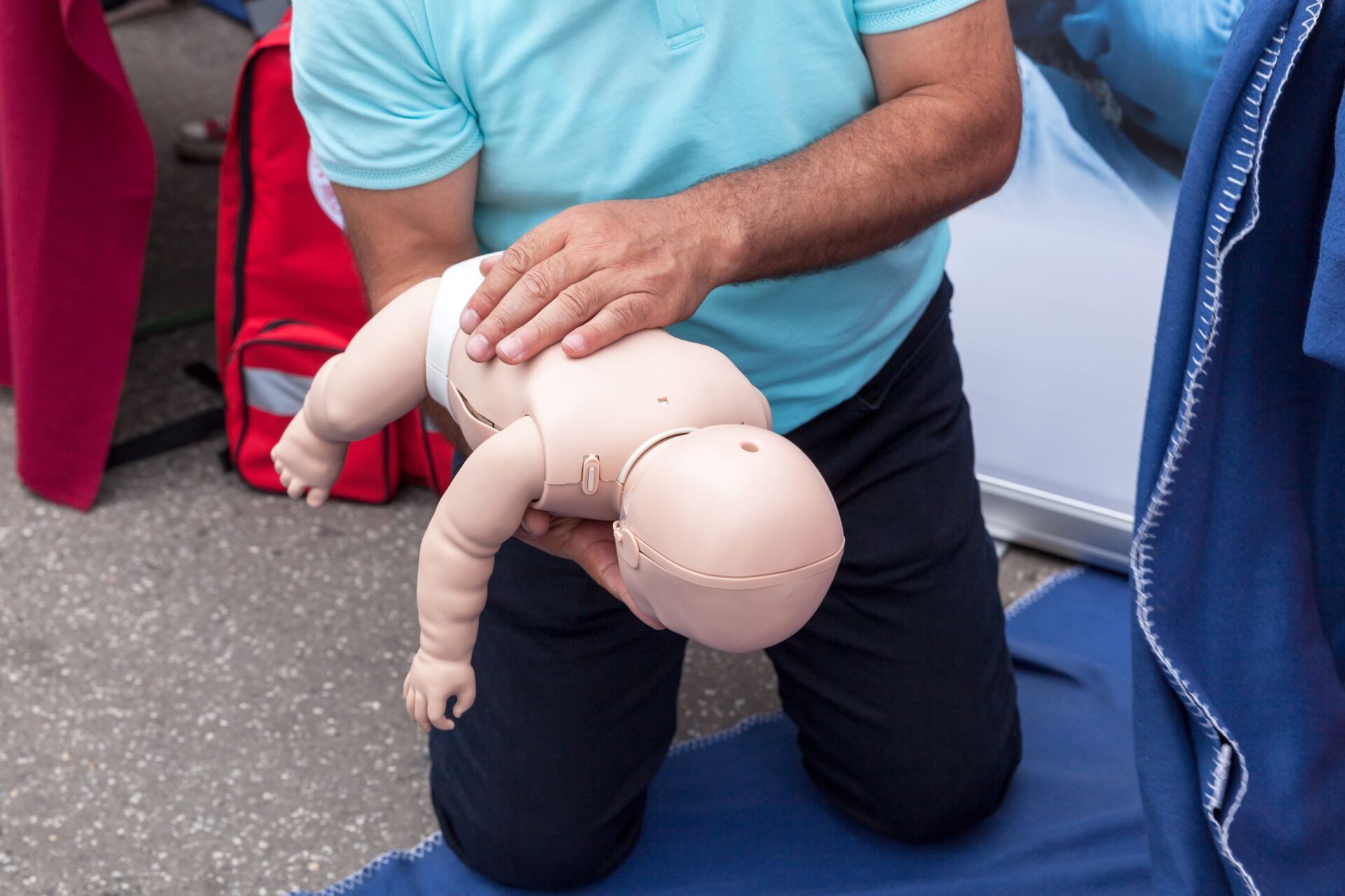
- Sandwich the baby between your forearms, supporting the head.
- Turn the baby face-down with the head lower than the body.
- Lower your forearm onto your thigh. With the heel of your hand, deliver five firm back blows between the shoulder blades.
- If the object has not been dislodged, while still supporting the head, turn the baby face-up, with your arms supported on your thigh.
- Place two fingers on the middle of the chest just below the nipple line and push hard and fast at least 4 centimeters (1.5 inches) or 1/3 to 1/2 the depth of the chest five times.
- Repeat the five firm back blows in five chest thrusts until the object is coughed up, the baby starts to cry, breathe or cough, or he or she becomes unconscious.
- Continue until EMS personnel arrive.
- If the baby becomes unconscious, follow the steps for unconscious choking baby below.
UNCONSCIOUS CHOKING BABY (UNDER ONE YEAR)
Care
- Start chest compressions:
- Place two fingers on the middle of the nipple line
- Do 30 compressions. Push hard and push fast.
- Allow the chest to recoil after each compression.
- Give one rescue breath:
- Tilt baby’s head and lift the chin.
- Take a normal breath.
- Cover the baby’s mouth and nose with your mouth.
- Give one breath lasting one second, with just enough volume to make the chest start to rise.
- If the baby’s chest does not rise after the first breath, perform the head tilt/chin lift again.
- Attempt to give another breath. If your breath still does not go in, go to Step 6. If your breath does go in, give a second breath.
- When both breaths go in, and there is no obvious response to your breaths, start CPR sequence of 30 compressions and two breaths.
- Repeat the cycle of 30 compressions, then look in the mouth:
- Grasp the tongue and lower jaw and lift.
- If you do not see an object, return to Step 2.
- If you see an object, remove it. Turn the head to the side, slide your finger down the side of the cheek to the base of the tongue, and try to sweep the object out. When it is removed, return to Step 2.
- Continue CPR until:
- An AED arrives
- The scene becomes unsafe
- You become physically unable to continue
Note After you reposition the head and attempt to give a second breath once, you do not need to repeat the repositioning step between chest compressions cycles. If there is any change in the baby’s condition during the CPR sequence, stop and check the baby’s ABCs. And if there are two people who can assist present, they should alternate every five cycles (about 2 minutes).
CHOKING CHILD (1 TO 8 YEARS)
Note To determine if choking is mild or severe ask, “Are you choking?” If the child can speak, cough or breathe, it is mild choking.
Care
- Encourage the child to continue coughing and do not interfere. The obstruction might clear itself.
- If the child is unable to speak, cough or breathe, or is wheezing or making high-pitched noises, it is severe choking:
- Stand (or kneel for a small child) behind the child and wrap one arm diagonally across the child’s chest.
- Bend the child forward at the waist until the child’s upper airway is at least parallel to the ground.
- With the heel of your hands, deliver five firm back blows between the shoulder blades.
- If the object has not been dislodged, make a fist and place it just above the child’s belly button.
- Place your other hand over your fist and pull sharply in and up, doing five abdominal thrusts.
- Continue the cycle of five firm back blows and five abdominal thrusts until the object comes out or the child begins to breathe or cough or becomes unconscious.
- If the object comes out, ensure the child is able to breathe easily again.
- Provide continual care and seek medical attention
- If the child becomes unconscious:
- Support the child to the ground protecting the head and placed the child on his back. Recheck the child’s ABCs.
- Call EMS, get an AED and follow the steps for unconscious choking child on the next page.
Note To deliver effective back blows, you may need to stand behind and slightly to the side of the child rather than directly behind the child.
UNCONSCIOUS CHOKING CHILD (1 TO 8 YEARS)
Care
- Start trust compressions:
- Place the heel of one hand on the middle of the child’s chest. Place the other hand on top.
- Do 30 compressions.
- Allow the chest to recoil after each compression.
- Give one rescue breath:
- Open the airway using the head tilt/chin lift.
- Pinch the child’s nostrils closed.
- Take a normal breath.
- Cover the child’s mouth with your mouth.
- Give one breath lasting one second, with just enough volume to make the chest start to rise.
- If the child’s chest does not rise after the first breath, perform the head tilt/chin lift again, tilting the head farther back and attempt to give another breath.
- If your breath still does not go in, go to Step 6. If your first breath goes in, give a second breath.
- When both breaths go in, and there is no obvious response to your two breaths, start the CPR sequence of 30 compressions and two breaths.
- Repeat the cycle of 30 compressions, then look in the child’s mouth.
- Grasp both the tongue and lower jaw and lift.
- If you do not see an object, return to Step 2
- If you can see an object, remove it. Turn the head to the side, slide your finger down the inside of the cheek to the base of the tongue, and try to sweep the object out when the object is out of the child’s mouth, return to Step 2.
- Continue CPR until:
- An AED arrives
- More advanced care takes over
- The scene becomes unsafe
- You become physically unable to continue
Note: If your breath does not go in, go back to compressions. After you reposition the head and attempt to give a second breath once, you do not need to repeat the repositioning step between chest compression cycles. If there’s any change in the child’s condition during CPR, stop and check the child’s ABCs.
-
-
- Prenatal 101
- Breastfeeding and the First Three Months
- Starting Solids and the Toddler Years
- An Age-by-Age Guide to Sleep
- Family Nutrition
- Kids and Mental Health
- When Your Child is Sick
- Safety and First Aid
- Milestones, Checklists and Charts


 From the pages of the Baby & Child Care Encyclopedia: Chapter 8, Safety and First Aid
From the pages of the Baby & Child Care Encyclopedia: Chapter 8, Safety and First Aid